
August’s Topic of the Month – Coping with Itchy Rashes
 August 31st, 2016
August 31st, 2016 Nakita Cambow
Nakita Cambow Blog
Blog 0 Comments
0 Comments
Skin involvement is common in lupus, with 60-70% of people with lupus reporting some skin problem. The rashes seen in lupus can be specific in shape and pattern. Rashes caused by lupus may get better after a few days or weeks, but can last longer or even be permanent.
What are the different types of lupus rash?
There are many different skin manifestations in lupus, which vary from person to person. Practically any type of rash can occur in lupus, ranging from widespread mild rashes similar to those seen in viral illnesses such as German measles, to small, distinct patches of rash on the elbows and knees resembling another skin condition, psoriasis. Rashes caused by lupus can sometimes be itchy or painful.
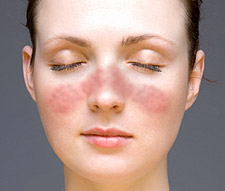 1. The ‘classical’ skin problem in lupus is the butterfly rash (otherwise called a malar rash). This is a red rash, sometimes no more than a mild blush that occurs across the bridge of the nose and on the cheeks. It can appear as a blotchy pattern or completely red over the affected area, and can be flat or raised. The rash can be mild or severe but is not usually painful. It can be itchy if it is more like a rash than a blush and some patients even report a ‘hot’ feeling with more severe malar rashes. This type of rash tends to occur in the systemic form of the disease (SLE), where other organs in the body may also be involved.
1. The ‘classical’ skin problem in lupus is the butterfly rash (otherwise called a malar rash). This is a red rash, sometimes no more than a mild blush that occurs across the bridge of the nose and on the cheeks. It can appear as a blotchy pattern or completely red over the affected area, and can be flat or raised. The rash can be mild or severe but is not usually painful. It can be itchy if it is more like a rash than a blush and some patients even report a ‘hot’ feeling with more severe malar rashes. This type of rash tends to occur in the systemic form of the disease (SLE), where other organs in the body may also be involved.
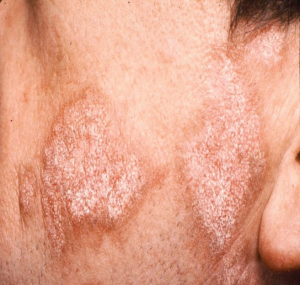 2. Chronic Cutaneous Lupus (also called discoid lupusor DLE) is only found in about 20% of people with SLE but can also be found in people with no trace of systemic lupus, in which case their lupus is generally confined to their skin only. These patches tend to be well defined, thickened and scaly; they are slightly red in colour and can itch. (The appearance can vary between individuals and also appear on different areas of the body on the same person). As the patches heal they tend to leave scars and in individuals with darker complexions the pigment can be lost, leaving white areas.
2. Chronic Cutaneous Lupus (also called discoid lupusor DLE) is only found in about 20% of people with SLE but can also be found in people with no trace of systemic lupus, in which case their lupus is generally confined to their skin only. These patches tend to be well defined, thickened and scaly; they are slightly red in colour and can itch. (The appearance can vary between individuals and also appear on different areas of the body on the same person). As the patches heal they tend to leave scars and in individuals with darker complexions the pigment can be lost, leaving white areas.
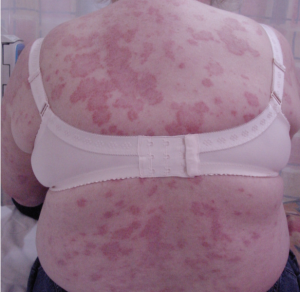 3. Subacute cutaneous lupus is a distinct rash that usually occurs in sun exposed areas of the body. It starts as scaly patches which increase in size to form circular areas, which gradually heal up, usually without leaving scars.
3. Subacute cutaneous lupus is a distinct rash that usually occurs in sun exposed areas of the body. It starts as scaly patches which increase in size to form circular areas, which gradually heal up, usually without leaving scars.
“I started having rashes on my skin and scalp and was back and forth to the doctor and given various diagnoses. Eventually I got referred to dermatology and after a skin biopsy, I got diagnosed with lupus. In some way it was a relief because I knew something wasn’t right.”
What causes itchy rashes in lupus?
Lupus flares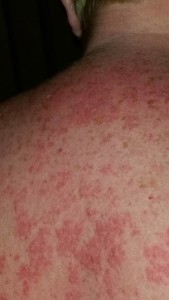
A flare is when someone has;
- a worsening of lupus symptoms
- a problem that was under control which comes back, or
- a new problem occurs that was not present before.
–
The development or exacerbation of a rash could be signs of a lupus flare. Often, flares may occur with no discernible reason. Some common causes of flares include not being diligent with wearing sunscreen, not avoiding ultraviolet light, stress, viruses, hormone fluctuations, not taking medications regularly, or even smoking cigarettes. If you can identify a potential cause for a flare, then it may help you learn to work on that particular aspect of your medical care/lifestyle and perhaps reduce the risk of it happening again.
“During the past few years whenever I get a virus of any sort I tend to get a rash all over my body (except for limbs) that looks a bit like sunburn. It disappears after 48 hours and can be slightly itchy.”
Exposure to sunlight/UV
 UVA-2 and UVB rays damage the cells of the skin (keratinocytes) and cause sunburn, skin aging and skin cancer. When these cells are damaged by the UV light it causes them to die. In healthy people without lupus, these dead cells are cleared away quickly and any inflammation caused by the sun-induced skin damage is short-lived (sunburn). However, in people with lupus, the skin cells may be more sensitive to sun-induced damage and there is increasing evidence that the dying (apoptotic) cells are not cleared away efficiently. As a result the contents of the dying cells may be released, including those found in their nuclei. These nuclear proteins (also called nuclear antigens) are particularly responsible for interacting with the immune system of a person who has lupus (especially with the famous antinuclear antibodies of lupus), encouraging it to become more active and cause inflammation and damage to various parts of the body.
UVA-2 and UVB rays damage the cells of the skin (keratinocytes) and cause sunburn, skin aging and skin cancer. When these cells are damaged by the UV light it causes them to die. In healthy people without lupus, these dead cells are cleared away quickly and any inflammation caused by the sun-induced skin damage is short-lived (sunburn). However, in people with lupus, the skin cells may be more sensitive to sun-induced damage and there is increasing evidence that the dying (apoptotic) cells are not cleared away efficiently. As a result the contents of the dying cells may be released, including those found in their nuclei. These nuclear proteins (also called nuclear antigens) are particularly responsible for interacting with the immune system of a person who has lupus (especially with the famous antinuclear antibodies of lupus), encouraging it to become more active and cause inflammation and damage to various parts of the body.
All forms of skin rashes in lupus are made worse by exposure to light (particularly sunlight). You can learn more about light sensitivity in lupus and how to protect yourself HERE.
“Stay out of the sunshine. Even total sunblock doesn’t stop me coming up in itchy red blobs!”
“I get itchy lupus rashes everywhere from the sun. I try to avoid it at all costs, but with two young children I do have to spend time outdoors. I can flare up from even ten minutes in my garden. My back and chest used to be the worst but now my arms and hands and knees seem to be the target. I also have it on my forehead most of the summer; it takes weeks to heal and leaves scarring on my face which darkens as soon as the sun hits it again.”
Sjögren’s syndrome
About one third of people with SLE will also have secondary Sjögren’s Syndrome (SS). SS causes inflammation and damage to the exocrine glands, which secrete fluids through tubes (called ducts), to the outside of the body. Along with causing dry eyes and dry mouth, SS can also affect the skin too when the sebaceous and sweat glands that secrete oils and sweat are affected. When the skin becomes dry due to decreased sweat and oil production it often becomes itchy as well. This can become especially apparent in the wintertime when the artificial indoor heat makes the dry winter air even drier.
The itchiness of the skin can sometimes be quite intense, even causing difficulty sleeping at night. The scratching of the skin while trying to alleviate the itching can cause irritation and inflammation of the skin, as well as the development of red patches on the skin. It is not uncommon for people to complain of itchy skin, not realising very dry skin is the cause.
You can learn more about Sjögren’s Syndrome at the British Association of Sjögren’s Syndrome (BSSA) website HERE.
What is the best way to cope with itchy rashes?
Treatment
The great majority of cases, even with severe skin involvement, can be controlled with a combination of effective protection against UV light, the use of topical corticosteroids and anti-malarial treatments.
Topical treatment
Locally applied corticosteroids can be very effective if the area of affected skin is not too large. These preparations vary in their strength from mild to very strong. Strong steroid preparations are often needed to begin with, but these should always be used under medical supervision because of the risk of skin damage.
“I use Betnovate on my hands and arms very sparingly and it clears it overnight. I was given this 45 years ago and it still works for me today with no thinning of my skin. For my dandruff I use glycerin rubbed into my scalp and left overnight. It feels greasy but it is water soluble and clears it away. It also helps with my skin but it has a tacky feel to it.”
Oral treatment
 Only very rarely is it necessary to resort to steroids or immunosuppressive agents by mouth for skin disease on its own. However, if topical treatment (usually creams and ointments) fails, or if skin involvement is too extensive, tablet treatment may be needed.
Only very rarely is it necessary to resort to steroids or immunosuppressive agents by mouth for skin disease on its own. However, if topical treatment (usually creams and ointments) fails, or if skin involvement is too extensive, tablet treatment may be needed.
Antimalarial drugs are usually very effective, as they help to reduce inflammation and the severity of the rash. Hydroxychloroquine is often well tolerated and usually does not cause any major side effects. It is advised to have yearly eye checks with an optician as hydroxychloroquine may rarely affect vision.
Thalidomide can be effective in difficult cases, but pregnancy must be avoided and a watch should be kept for side effects such as nerve damage, which may give rise to tingling in the fingers.
All drugs have the potential to cause side effects and the prescriber’s responsibility is to balance the potential risks of the drug against the potential benefits and the risks of leaving the condition untreated (which may be more harmful in the longer term). Always discuss any concerns you may have about medication with your doctor or nurse so that you can make an informed decision about what you are being prescribed.
Avoiding sunlight/UV
 People who are sensitive to UV light should avoid exposure to direct sunlight and wear a hat and long sleeves to provide a barrier. Sunscreens are also needed for exposed parts of the body. You should use a sunscreen that has an SPF of at least 50 and a four-star UVA rating. Your doctor can prescribe some sunscreens.
People who are sensitive to UV light should avoid exposure to direct sunlight and wear a hat and long sleeves to provide a barrier. Sunscreens are also needed for exposed parts of the body. You should use a sunscreen that has an SPF of at least 50 and a four-star UVA rating. Your doctor can prescribe some sunscreens.
Learn more tips for protecting yourself from UV HERE.
“I use factor 50 which prevents the rashes on my body but I still get them on my face. To calm my face down I use Bepanthen nappy rash cream which kills the itch really well.”
“I use a factor 50 sunscreen and bought a special factor 50 shirt and a hat which I wear when gardening to protect me from the sun.”
Treating dry skin
If your itching is caused by dry skin (perhaps as a result of Sjögren’s syndrome), you may want to follow some of the advice below;
- Drink plenty of fluids, especially water throughout the day.
- Avoid dehydrating fluids such as alcohol and caffeine.
- Avoid smoking.
- Use a humidifier in each room of your house where you spend significant time, especially the bedroom. Keep the air humidity about 50%. Clean and dry out humidifiers daily to prevent mould and fungus.
- Do not use soap on most body surfaces, except underarms and private areas, more than a couple of times per week. Soap removes natural, lubricating oils from your skin.
- Use an oil-based soap instead of other soaps (even those that claim to contain moisturisers).
- Shower or bathe in lukewarm water, not hot water. Hot water removes the natural, lubricating oils from your skin. Whatever your bath or shower temperature is currently, make it slightly cooler (the cooler the better).
- Take shorter baths and showers.
- After bathing or showering, pat the skin dry; do not rub as this removes moisturising oils.
- Apply a moisturiser to dry body areas immediately after bathing.
- Use a heavy-duty moisturiser that contains urea, glycerine, lactic, or alpha hydroxyl acids.
- Consider moisturisers that contain ceramides, which can help repair the skin’s protective barrier.
- For areas of very dry skin, consider using petrolatum (Vaseline) or bath oil right after you bathe and while your skin in still moist (to trap moisture in the skin).
- Reapply a moisturiser several times a day.
- Avoid using fabric softeners as they can irritate dry skin.
–
“My mum found that soapy products were the worst. She took a tip from my daughter’s eczema routine and started to use the Simple range. She found it a lot better. Oilatum also locks in moisture and prevents the skin drying out.”
“Mix bicarbonate of soda with water to make a paste, then dab it on the rash.”
“I’ve bought some vitamin E gel from QVC from the SBC beauty range. It’s made my skin calm down completely and the smell is lovely, which makes me want to use it.”
“[I use] Aloe Vera gel. I wash my skin which has been exposed to the sun when I come in (to cool it), then I apply the gel or M&S’s Aloe and Mint Hand and Body Lotion. I used it this holiday and love it.”
“[I have a] lukewarm shower followed by the Protopic ointment and Diprobase creams. If it’s really bad I take antihistamines too.”
“[I use] Aloe Vera gel and calamine lotion daily. I moisturise well at night, take a daily antihistamine and avoid sunlight (which triggers the rash). I use steroid cream if it gets bad (but I haven’t needed to use it for a long time).”
“Cooled peppermint tea bags or cucumber mashed and placed in the fridge.”
“A few drops of lavender oil in a bath or in a water spray to use as required are good for calming an itch.”
“Natural yogurt or an oatmeal bath.”
“I use coconut oil with vitamin E or sesame oil. My skin was terrible and very dry, but now it’s perfect. It is not expensive and it works fine for me. When the skin looks fine already you can use aloe vera gel as well. I usually react badly to everything.”
***Please note that this article is written for informational purposes only and should not be a substitute for professional medical advice or treatment. Do not delay seeking or disregard medical advice based on information here. Always seek the advice of your local family physician or other qualified health professional before starting any new treatment or making any changes to existing treatment. It is also advisable to consult a medical professional before making any changes to diet or starting alternative remedies, which may interact with other medications.***
Thank you so much to everybody who submitted their tips and experiences for this month’s topic. We’re sorry if we weren’t able to use your comment in the article this time.



 ©2024 LUPUS UK (Registered charity no. 1200671)
©2024 LUPUS UK (Registered charity no. 1200671)