
October’s Topic of the Month – Coping with Raynaud’s Phenomenon
 November 02nd, 2016
November 02nd, 2016 Nakita Cambow
Nakita Cambow Blog
Blog 0 Comments
0 Comments
Raynaud’s phenomenon is a common problem that occurs in the cardiovascular system of people who have lupus, appearing in approximately one-third of cases.
What is Raynaud’s phenomenon?
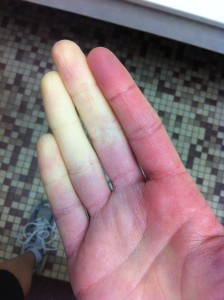 Raynaud’s phenomenon is named after the French physician Maurice Raynaud who first described Raynaud’s phenomenon in a young woman in 1862. In people who have Raynaud’s, the small blood vessels in the extremities are over-sensitive to changes in temperature. This causes a Raynaud’s attack where the fingers sometimes change colour (but not always) from white, to blue, to red. Sometimes the fingers may become painful or have a tingling sensation during the event. Symptoms of a Raynaud’s attack can last from a few minutes to several hours.
Raynaud’s phenomenon is named after the French physician Maurice Raynaud who first described Raynaud’s phenomenon in a young woman in 1862. In people who have Raynaud’s, the small blood vessels in the extremities are over-sensitive to changes in temperature. This causes a Raynaud’s attack where the fingers sometimes change colour (but not always) from white, to blue, to red. Sometimes the fingers may become painful or have a tingling sensation during the event. Symptoms of a Raynaud’s attack can last from a few minutes to several hours.
“My hands in particular can be so bad I can’t go into a shop with air conditioning or get something out of the fridge (I have to wear thermal gloves for the freezer). Over the last couple of years my nose is suffering a lot.”
“Sometimes simply holding metal cutlery will set my hands off, or walking down a supermarket freezer aisle!”
“My fingers will go as soon as the temperature drops from hot/warm to a few degrees cooler, whether that’s just getting out of bed, moving from one room to another or going outside and just moving from warm sun to slightly cooler shade in the summer.”
“Don’t forget nipples! I’m a breastfeeding mum and it came as quite a shock to me when I got this.”
What causes Raynaud’s phenomenon in lupus?
Whenever someone is exposed to cold temperatures, the nerves of the skin, blood vessels, and brain sense the colder temperature and then send chemical messages along the nervous system to the arteries of the skin, hands, and feet, telling them to constrict to keep as much warm blood as possible away from the skin, fingers, and toes. This helps to prevent the body from losing vital warmth through the skin, and to keep the blood and inner part of the body (with vital organs like the brain, kidneys, and heart) at the correct warm body temperature. In the vast majority of people, this chain of events just causes the skin to feel cooler than normal.
However, in a person who has Raynaud’s the flow of blood is restricted so much that less reaches the extremities. Since there is less blood flow, the fingers and toes (and sometimes the ears and nose) may become pale and colder than normal. Then, as the tissues and cells use up the oxygen and release more carbon dioxide into the blood, this causes the normally red blood to become blue or purple. With rewarming, there may be reddish colouration as more fresh blood flows in.
The restricted blood flow in Raynaud’s may be the result of damage accumulated by inflammation from lupus. Inflammation can cause the walls of the arteries to be thicker than normal and therefore the arteries in the body’s extremities have a smaller than normal inner channel through which blood flows.
What are the potential complications of Raynaud’s?
 In some cases, after repetitive episodes of Raynaud’s, the tissues of the fingertips may not have enough nutrients and oxygen to remain normal. Over time, the fleshy parts of the fingertips (on the palm side) may lose tissue and become tapered and thin instead of staying plump. In more severe cases, blood flow may be so restricted during the episodes that the tissue on the fingertips may actually die due to the lack of nutrients and oxygen. This can potentially cause open sores to develop. These can be very painful and are prone to infection if not treated. Trauma to the fingertips, even minimal trauma, appears to increase the possibility of this happening.
In some cases, after repetitive episodes of Raynaud’s, the tissues of the fingertips may not have enough nutrients and oxygen to remain normal. Over time, the fleshy parts of the fingertips (on the palm side) may lose tissue and become tapered and thin instead of staying plump. In more severe cases, blood flow may be so restricted during the episodes that the tissue on the fingertips may actually die due to the lack of nutrients and oxygen. This can potentially cause open sores to develop. These can be very painful and are prone to infection if not treated. Trauma to the fingertips, even minimal trauma, appears to increase the possibility of this happening.
“I suffer badly with this in my hands and feet and have had severe chilblains on my toes in the winter since I was a teenager.”
The thickened blood vessel walls that cause Raynaud’s are usually the result of previous inflammation and are a permanent problem. Therefore Raynaud’s usually does not get better over time and does not improve with the use of anti-inflammatory medicines such as steroids and immunosuppressant medicines. Raynaud’s does not usually vary between lupus flares and remissions.
Secondary Raynaud’s (when it’s caused by another health condition, such as lupus) can severely restrict the blood supply, so it carries a higher risk of complications, such as ulcers, scarring and even tissue death (gangrene) in the most serious cases. However, severe complications are rare. You can read more about the complications of Raynaud’s HERE.
“Keeping my hands moisturised is really important to try and prevent cracks in the skin, which I tend to get in the winter. These cracks in the skin are very sore and very painful when the blood drains away from them.”
How is Raynaud’s phenomenon diagnosed?
 If you suspect that you may have Raynaud’s, speak to your GP in the first instance.
If you suspect that you may have Raynaud’s, speak to your GP in the first instance.
A cold stimulation test can be used to trigger Raynaud’s symptoms. For this test, a small device that measures temperature is taped to your fingers. Your hands are then exposed to cold – a one minute immersion in cold water at 15⁰C.
Your hands are then removed from the cold, and the device measures how quickly your fingers return to their normal temperature. If you have Raynaud’s, it may take more than 20 minutes for your fingers to return to their normal temperature. Because results of this type of test are not always consistent, your doctor may do other tests to check for Raynaud’s.
Your GP may also check the tiny blood vessels, known as capillaries, found where your nail meets the finger. These capillaries are often larger in people with secondary Raynaud’s, and look like red pen marks.
“The cold water test isn’t 100% accurate because for some people the whole body has to be cold to cause an attack. The best way to get diagnosed is by taking pictures of what happens to you when you get cold.”
How can I manage my Raynaud’s?
Although there is no cure for Raynaud’s, it can be treated. The key to managing Raynaud’s symptoms is to try to prevent an attack, so planning ahead is essential.
Symptoms can be triggered by mild changes in temperature (such as taking an item out of the fridge or freezer) or sometimes strong emotions such as stress or anxiety. It is very important for people who have Raynaud’s to keep the core body temperature warm and to avoid potential triggers for attacks.
“My Raynaud’s tends to flare during moments of excitement as well. I’m happy, received great news . . .and now I have blue hands!!!”
“One of the most important things I have to make sure I do is to be warm before I leave the house.”
“The trick to prevent attacks is by wearing layers and finding a funky hat to keep 30% of our body heat in!”
“I find that I need to keep my core warm – longer tops, tucked in if possible to stop the cold getting in!”
Here are some ways that you can try to manage your Raynaud’s symptoms;
- Avoid cold places

- Wear layers of clothing in cold temperatures
- Wear mittens, which are preferable to gloves
- Wear gloves/mittens to touch frozen or cold foods
- Wear heavy wool stockings
- Wear a hat in cool temperatures
- Keep hand-warmers in your pockets
- Wear battery-heated gloves
- Avoid air conditioning
- To stop a Raynaud’s attack, rub your hands together, run them under warm water, put them under your armpits, or whirl your arms around like a windmill to increase blood flow to your hands
- Avoid vibrating tools, which can worsen Raynaud’s
- Do not smoke cigarettes (nicotine constricts blood vessels)
- Avoid caffeine (caffeine constricts blood vessels)
- Avoid taking decongestants, amphetamine-like diet pills, and herbs containing ephedra (all these constrict blood vessels)

- Protect your fingertips to prevent sores from occurring
- Biofeedback therapy can train the brain to learn to keep the blood vessels more relaxed and open
- Take rests when you can to avoid getting too fatigued
- Try to steer clear of stressful situations as stress and anxiety can trigger an attack1
- Take gentle exercise2
–
1For more advice about managing stress, visit the NHS Choices page HERE.
2Exercise, within your own limits, can boost circulation and may improve Raynaud’s. Even very gentle exercise can help to get the blood flowing – if you are feeling cold, for example, try swinging your arms as you walk.
Occasionally, exercise can trigger Raynaud’s attacks. Look out for signs of this happening and change your routine if necessary. Many find swimming can help their Raynaud’s, but it is important to check the temperature of the water before swimming, as a cold pool could trigger an attack.
For more advice about lupus and exercise, please have a look at our previous blog article HERE.
“For the freezer I wear gloves to take anything out. I can’t handle veg etc. that has just come out of the fridge or use cold water for cleaning these.”
“After the shower I dry myself with a hair dryer to warm up quickly.”
“I keep a portable heater in the bathroom. It’s a great help in the winter months.”
“My hint for when in the shower or the bath; use exfoliating gloves and rub in circles from the feet up; this aids the circulation. You should always rub towards the direction of your heart; with legs go from the bottom to the top, and with arms from the wrist to the shoulder. This gives your circulation a good boost and does wonders for restless legs. Also when drying with a towel, scrub instead of patting using circular motions towards the heart.”
“Blankets, socks, gloves, etc. actually tend to insulate your hands and feet with cold if they start out cold (much like a thermal glass will keep a cold drink, cold and hot one, hot). Some outside source or other body part must make them warm first. Then add coverings to keep the warmth in as long as possible.”
“When my husband and I hold hands, I can’t let him hold mine, I have to hold his. Otherwise, the squeezing, even lightly, cuts the flow. We definitely cannot cross fingers!”
Products that may help
Scleroderma & Raynaud’s UK’s shop includes a range of different insulated and heated products to help you manage your condition. Have a look at the range available HERE.
Here are some suggestions we have received from people with lupus and Raynaud’s;
“I couldn’t live without my sheepskin boots/slippers, as they are the only things that keep my feet warm throughout the cold months. Soft leather fleece-lined gloves for driving and padded thermal mitts for anywhere else, I definitely couldn’t live without any of these products.”
“I wear colour-changing nail varnish so I can keep a visual check on the temperature of the tips of my fingers and go run them under warm water when I need to. I buy it from Amazon. It’s UV-cured nail varnish (I have a lamp, and it doesn’t make me react like the sun does, so it seems to be ok for me to use).”
 “I have invested in an electric blanket as my feet are always cold. I switch it on before bed and then it takes me around 20 minutes to warm my feet. I then switch it off.”
“I have invested in an electric blanket as my feet are always cold. I switch it on before bed and then it takes me around 20 minutes to warm my feet. I then switch it off.”
“Try a furry steering wheel cover; it doesn’t stop the cold completely but it does help.”
“I use the gel hand warmers inside thermal or sheepskin mittens, not gloves (fingers seem to stay warmer when they’re all together).”
“I work on a PC all day and find my fingers go icy so I wear fingerless gloves in the office to help combat that. I found some which plug into the PC base station via an Ethernet lead and are heated; just gentle warmth.”
“Hand warmers are great while stood watching my son’s football team on cold mornings. You can get them in loads of place – pound shops sell them too. Click the silver disc and they heat up instantly for 1hr-1.5hrs. Boil them and then they are re-usable.”
“Uniqlo do heat generating thermals that are incredibly thin so great for layering – I often wear two of their tops under fleeces.”
“The best thing I have ever done was buy myself a water bed. It is heated and kept at a constant temperature so I’m lovely and warm all over at night and also it has really improved my sleep pattern as I now don’t wake up several times a night not being able to move because my joints hurt so much.”
Are there any treatments for Raynaud’s?
 Allowing mild Raynaud’s attacks to occur is acceptable as long as they are not painful, fairly easy to control, and do not cause the loss of tissue in the fingertips or open sores. However, if the attacks are not mild, then treatment by medication may be necessary.
Allowing mild Raynaud’s attacks to occur is acceptable as long as they are not painful, fairly easy to control, and do not cause the loss of tissue in the fingertips or open sores. However, if the attacks are not mild, then treatment by medication may be necessary.
One drug, nifedipine, a calcium channel blocker, is licensed for Raynaud’s, and there are other drugs that are prescribed commonly for Raynaud’s too. Some of the medicines used in the treatment of Raynaud’s were originally developed to treat other disorders (such as hypertension, depression, angina, or erectile dysfunction).
“I have Raynaud’s phenomenon and I couldn’t manage without taking nifedipine daily.”
“My doctor prescribed Adalat [nifedipine] which has really helped as it helps open up the blood flow to the extremities.”
Studies show that the antidepressant fluoxetine is helpful in some people. Other treatments could include nitroglycerin, sildenafil (Viagra) and some people may benefit from a low dose of aspirin daily.
Other treatments could include;
- Iloprost infusions (in extreme cases of Raynaud’s)
- Botox (this is an experimental Raynaud’s treatment, which may reduce blood vessel spasm and block pain nerves. Increasing amounts of research is emerging for it, but it is only used in selected cases and usually only in specialist centres)
- Acupuncture (some Raynaud’s sufferers have found this can alleviate symptoms)
_
For particularly severe, resistant cases of Raynaud’s, measures that are more drastic may be necessary, such as sympathectomy – a surgical procedure in which a surgeon cuts the sympathetic nerves to the hands. In addition, a doctor can inject an anaesthetic around the nerves (called a sympathetic nerve block) to keep them from causing the constriction of blood vessels.
For more information about Raynaud’s phenomenon you can visit the Scleroderma & Raynaud’s UK website or download their factsheet- HERE
***Please note that this article is written for informational purposes only and should not be a substitute for professional medical advice or treatment. Do not delay seeking or disregard medical advice based on information here. Always seek the advice of your local family physician or other qualified health professional before starting any new treatment or making any changes to existing treatment. It is also advisable to consult a medical professional before making any changes to diet or starting alternative remedies, which may interact with other medications.***
Thank you so much to everybody who submitted their tips and experiences for this month’s topic. We’re sorry if we weren’t able to use your comment in the article this time.




 ©2024 LUPUS UK (Registered charity no. 1200671)
©2024 LUPUS UK (Registered charity no. 1200671)