
November’s Topic of the Month – Getting the Most from your Medical Appointments
 December 06th, 2016
December 06th, 2016 Nakita Cambow
Nakita Cambow Blog
Blog 0 Comments
0 Comments
One of the most important ways to manage your lupus is to be an active member of your own healthcare team. Research has shown that patients who have good relationships with their doctors tend to be more satisfied with their care – and to have better results.
A good patient–doctor relationship
 Your relationship with your doctor is an important partnership that can last for many years. You and your doctor work together to manage your medical conditions and achieve the best result for your health that is possible. A good doctor-patient relationship includes mutual trust, respect and good communication. You may be able to improve the quality of your care by helping the doctor develop the best understanding possible of your symptoms and condition(s).
Your relationship with your doctor is an important partnership that can last for many years. You and your doctor work together to manage your medical conditions and achieve the best result for your health that is possible. A good doctor-patient relationship includes mutual trust, respect and good communication. You may be able to improve the quality of your care by helping the doctor develop the best understanding possible of your symptoms and condition(s).
“I’m blessed with a wonderful GP and a great consultant rheumatologist. It helps to prepare for the hospital appointments by emailing issues to my rheumatologist’s secretary the week before.”
If you do not have a good relationship with your doctor and feel that the only way to improve things is to see another doctor who may communicate better, respect you more, or partner with you more effectively then it may be the wisest course to change your doctor – you can read more about this further down.
A visit to your GP or consultant can be intimidating and cause anxiety but there are practical measures you can take to alleviate some of this stress and get the most out of your appointments;
Preparation – Before Your Appointment
 Whether it is your initial GP appointment, a consultation with a specialist at an outpatient appointment or a mental health assessment there are a few things you can prepare in advance that will help you to get the most out of your time with the health professional.
Whether it is your initial GP appointment, a consultation with a specialist at an outpatient appointment or a mental health assessment there are a few things you can prepare in advance that will help you to get the most out of your time with the health professional.
Each doctor only has a certain amount of time allotted to each patient appointment. The amount of time allotted depends a lot on the doctor, the specialty, the types of problems they see, and the average amount of time most problems take to address. By being prepared before the appointment you will be able to make the most of the time available. If you have a complicated problem, ask for a longer appointment when you book.
“I’ve learned that the success (or otherwise) of consultations usually depends on being really well prepared in every possible way.”
Is your issue urgent?
Is it important you are seen quickly or would you rather wait for an appointment with a particular GP? There may be times when you could benefit from seeing a GP who knows your history personally, but other times you may need a symptom investigated more urgently. If you feel you need urgent medical care and no GPs are available it may be best to go to your nearest walk-in centre or A&E.
“When I get something wrong with me I get an appointment straight away as with lupus things come out of the blue. One day you can be ok and the next day you can have a really bad chest; so deal with the problem as soon as possible.”
“Make it a priority to find a sympathetic, supportive GP, and see only them if you can. I kept seeing whoever was available on the day, and it drove me mad.”
Make notes
 Before your appointment, you should already have in mind what your goals are for the visit. Pick out your top three most important concerns and write them down. Try your best to be brief in phrasing any questions. You can hand this list to your doctor at the very start of the visit to allow them time to read them and plan them into the appointment. It is important not to list every single problem that you can think of, as digesting the information is likely to take too much of the allotted time and your doctor is unlikely to be able to solve all your concerns in one visit. If you are unsure what to ask your doctor, a useful list of questions can be found HERE.
Before your appointment, you should already have in mind what your goals are for the visit. Pick out your top three most important concerns and write them down. Try your best to be brief in phrasing any questions. You can hand this list to your doctor at the very start of the visit to allow them time to read them and plan them into the appointment. It is important not to list every single problem that you can think of, as digesting the information is likely to take too much of the allotted time and your doctor is unlikely to be able to solve all your concerns in one visit. If you are unsure what to ask your doctor, a useful list of questions can be found HERE.
“Make a list of things you want to ask beforehand; just the most important ones first. If you don’t write it down it’s easy to come out and remember something you forgot to ask.”
“Plan your appointment, take a list if necessary. Don’t say general things like, ‘I hurt all over’. Describe your symptoms clearly (e.g. muscles in upper arms and thighs ache). Instead of saying, ‘all my joints’, say ‘my fingers, shoulders hips etc. are swollen, hot and painful’. Doctors tend to listen to more specific descriptions than general ‘I feel awful’ type statements. Describe why you feel awful (fatigue is debilitating etc.)
I usually have an A4 list, but it is split into three sections; new symptoms, ongoing symptoms (such as fatigue and joint pain), and any changes or improvement since the last visit. I begin with the symptoms that trouble me the most/ cause me the most pain. It’s important to let the consultant see the list as they may make connections that we haven’t seen.”
If you are seeing a specialist consultant, when picking the most important problems it is important to consider whether they are problems that this particular specialist can handle.
Keep some abbreviated medical records with you (one or two pages listing the names and contact numbers of your doctors, what medical problems you have, any surgery you may have had, allergies, changes in any medicines by other doctors and new medical problems since your last visit).
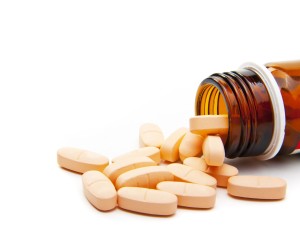 It is also important to keep a complete list of your medications (or bring all your pill bottles/boxes to every visit). It is important to never assume that the medication list in your records is correct. Your list should include all medications you are taking, including over-the-counter and/or alternative/complementary medicines; this includes tablets, liquids or creams.
It is also important to keep a complete list of your medications (or bring all your pill bottles/boxes to every visit). It is important to never assume that the medication list in your records is correct. Your list should include all medications you are taking, including over-the-counter and/or alternative/complementary medicines; this includes tablets, liquids or creams.
“I had such severe rashes I took photos on my iPad and brought it along on my last appointment. It’s better than just saying ‘I’ve had a rash’. My doctor was surprised how bad it was.”
Give yourself sufficient time
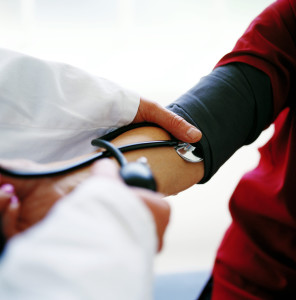
Aim to arrive at least fifteen minutes early for your appointment. This will allow time for any delays or heavy traffic on your journey and if you arrive early, you will be calm and your blood pressure should be reliable when measured.
Dress appropriately
If the appointment will include a physical examination of a symptom it can save time by dressing so that the area can be accessed easily. Obviously it is important to ensure that you still dress appropriately for the weather outside.
Summary
- Write down your two or three most important questions/concerns.
- List or bring all your medicines and pills – including vitamins and supplements.
- Write down details of your symptoms, including when they started and what makes them better or worse.
- Ask your hospital or surgery for an interpreter or communication support (if needed).
- Ask a friend or family member to come with you (if this helps).
- Allow plenty of time and aim to arrive for your appointment early.
- Dress appropriately.
–
“Be persistent. Only once your GP realises that they’ve seen you a lot recently will they start to understand that you’re not there because you want to be. I have a great GP and hospital team now but my last GP surgery were hit and miss.”
“If you don’t feel confident take a supportive partner/friend along”.
During the Appointment
Hand the doctor your list of most important questions and concerns at the very beginning of the visit (remember, your doctor is on a very tight schedule).
Giving information
 Around 80% of the information your doctor needs to make a correct diagnosis comes from what you say to him/her. The remaining pieces of the puzzle are found when you are examined and have tests carried out. This verbal information, ‘the history’, is very important and is mostly obtained in two ways – the first is when you answer your doctor’s questions, the second is when you say things without being asked.
Around 80% of the information your doctor needs to make a correct diagnosis comes from what you say to him/her. The remaining pieces of the puzzle are found when you are examined and have tests carried out. This verbal information, ‘the history’, is very important and is mostly obtained in two ways – the first is when you answer your doctor’s questions, the second is when you say things without being asked.
It is in your best interest to answer all questions asked by your doctor completely and truthfully. Be honest about what you think may be causing a problem, and don’t be embarrassed; your doctor will have seen and heard it all before. Even what seem to be very personal questions may be very important to your medical condition. If you do feel uncomfortable, just be honest and say so rather than giving a false answer. Also, let the doctor know if you are not taking your medications as prescribed. If you take something just when you feel you need it, or if you are not taking it (for any reason), it is extremely important to let your doctor know that.
It is important not to understate your symptoms or how difficult you may be finding it to manage. It’s hard enough for anyone who is not battling a chronic illness like lupus to understand when you may not look sick.
“If you’re anything like me, it is important to emphasise as honestly as you can, how much pain or fatigue are affecting/ impacting on your daily life and work. I tend to forget to do this because I find it awkward or embarrassing – but when I’ve done it the doctor has usually opened their eyes wider and thought harder about me from this moment on.”
Patients are much more educated today than ever before, largely because of the internet. However, the internet is a double-edged sword as there is a lot of medical misinformation out there as well. Becoming focussed on one possible diagnosis without allowing your doctor to consider all possibilities can be detrimental if you don’t have an open mind. A good approach may be to let your doctor know what your worry is instead of insisting you have a particular disease/condition.
Asking questions
Don’t be afraid to ask if you don’t understand something that the doctor has explained. If you don’t understand any words or terms that they use, ask for them to be written down and explained. Also by having them written down, you can look them up later if necessary.
“Don’t feel afraid to challenge the doctor or say things like, ‘I don’t like the way you are making me feel’ or ‘I don’t feel you are listening or understanding’. Sometimes we just have to fight some more.”
Take notes
It can be helpful if you (or a family member or friend with you) take notes during the appointment. This can allow you to tick off items on your list as you go along, write down any words or terms that you may want to look up in more detail later, and remember any instructions given by the doctor. Making notes can be especially helpful if you experience brain fog.
“You can take notes. Take the email address or the telephone number from your consultant so you can call/email them about any concerns you have.”
Before you leave your appointment
Before you leave your appointment, it is important to ensure that you have achieved all of the goals that you decided beforehand. Be clear about what you want the doctor to do, such as refer you to a specialist or prescribe a different medication. Be assertive if you need to, but always be polite. If you and your GP decide you need to be referred for specialist tests or treatment, (if you live in England) you usually have a right to choose which hospital and/or consultant led-team you go to. You can read more about this HERE.
Check:
- You’ve covered everything on your list.
 You understand everything that has been explained to you. If you don’t fully understand, don’t be afraid to ask your doctor to go through everything again. For example you could ask, ‘Can I just check I understood what you said?’
You understand everything that has been explained to you. If you don’t fully understand, don’t be afraid to ask your doctor to go through everything again. For example you could ask, ‘Can I just check I understood what you said?’- You know what should happen next and when. Remember to make a note of it.
–
Ask:
- Who to contact if you have any more problems or questions.
- About support groups and where to go for reliable
information. - For copies of letters written about you – you are entitled to see these.
- What happens if you’re not sent future appointment details.
–
After your appointment
Keep records
It can be helpful to write down what you discussed in your appointment and what happens next. Keep your notes organised in case you need to refer to them before your next appointment (or at another point in the future).
Take any actions
 If you were asked by your doctor to book any tests or future appointments make sure you do this and put the dates in your diary/calendar.
If you were asked by your doctor to book any tests or future appointments make sure you do this and put the dates in your diary/calendar.
Request results
If you are awaiting test results and you don’t get them when you expect – ask for them. If you need help understanding what the results mean, ask your medical team to explain them to you.
Changing doctor
Mutual trust and respect are very important between a doctor and patient. If your doctor does not manage your expectations well, uses medical jargon, or fails to provide test results or other feedback, it is easy to get frustrated with communication problems. If this is the case, then it may indicate that changing doctors could be your best course of action. If you are considering making a change, don’t take the decision lightly; you and your doctor have both invested in the relationship, and such a change will not necessarily be easy.
Changing GP
If you’re not happy with your current GP, you can ask to see another doctor in the practice. You can also change GP practices, but you should discuss your concerns with a practice staff manager first.
You can change your GP at any time you wish without having to give a reason. If you tell your local Clinical Commissioning Group (CCG) that you want to change your GP, they must give you details of how to do so and provide you with a list of alternative GPs. You do not need the consent of your current GP. When you have found another GP willing to accept you, you should contact them and ask if they will take you on. You can then make an appointment to see the new GP immediately.
“See another GP!!! Mine was useless and for the first three years since my diagnosis, I could not get decent answers and care. I collapsed at work in January and was seen by a new female GP who has been amazingly supportive and knowledgeable; what a difference it makes! She works in the same practice and I am now registered with her. Don’t wait too long like I did; seek professionals who can help rather than dismiss or hinder you. I was not sleeping well and now thanks to being aware of it, I take medication and have had far less pain and am sleeping better. I suffered needlessly for over three years as the old GP had no clue”
Changing consultant
You can ask your GP, consultant or hospital unit for a second or further opinion (an opinion about your health condition from a different doctor). Although you don’t have a legal right to a second opinion, a healthcare professional will consider your circumstances and whether a second opinion is needed.
If you would like a second opinion after seeing a consultant, you can discuss this with them directly or with the hospital unit.
People living in England could also contact the hospital’s Patient Advice and Liaison Service (PALS) if you have any concerns or complaints. You can find your local PALS HERE.
People living in Scotland can contact the Patient Advice and Support Service. Learn more about this service and how to contact them HERE.
People living in Northern Ireland can contact the Patient and Client Council. Learn more about this service and how to contact them HERE.
People living in Wales can contact the Patient Support and Advisory Service. Learn more about this service and how to contact them HERE.
You’ll usually need to go back to your GP and ask them to refer you again. If your GP agrees to refer you to a new consultant, the consultant will be told that this is your second opinion. They’ll also be sent any relevant test results or x-rays previously carried out. This doesn’t mean the new consultant will automatically take over your care. If you want to be treated by the new consultant, this needs to be arranged with the doctors and hospital.
If you need information about consultants in your area who have a specialist interest in lupus, you can contact us. You can also ask other people with lupus for their recommendations on our HealthUnlocked forum or through our Regional Support Groups.
Thank you so much to everybody who submitted their tips and experiences for this month’s topic. We’re sorry if we weren’t able to use your comment in the article this time.



 ©2024 LUPUS UK (Registered charity no. 1200671)
©2024 LUPUS UK (Registered charity no. 1200671)