
March’s Topic of the Month – Pain Management
 April 04th, 2017
April 04th, 2017 Nakita Cambow
Nakita Cambow Blog
Blog 0 Comments
0 Comments
Chronic pain is very common in lupus. It can have a huge impact on your quality of life, and can also affect the lives of your family and those around you. There are various pain management techniques available that can hopefully help you to manage your pain better, making life more enjoyable and rewarding.
Causes of pain in lupus
Arthralgias and Myalgias
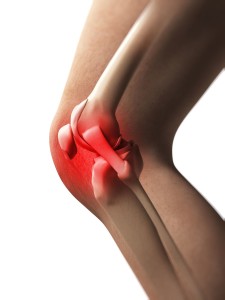 90% to 95% of people with lupus will experience muscle and/or joint pain. Arthralgias are pains in the joints, and myalgias are pains in the muscles. The ending “-algia” comes from the Greek word for “pain”. These pains will often be termed “polyarthralgias” and “polymyalgias” as well (“poly-“ means “many”). Experiencing arthralgias and myalgias does not necessarily mean that there is actual arthritis (actual inflammation or damage in the joints) or muscle inflammation. The doctor may not see any evidence of inflammation on examination. If a patient just has achy joints (arthralgias) without having actual inflammation of the joints (arthritis), doctors usually prescribe pain relievers for treatment. These include Paracetamol, non-steroidal anti-inflammatory drugs (NSAIDs; such as ibuprofen and naproxen), or other analgesics such as tramadol.
90% to 95% of people with lupus will experience muscle and/or joint pain. Arthralgias are pains in the joints, and myalgias are pains in the muscles. The ending “-algia” comes from the Greek word for “pain”. These pains will often be termed “polyarthralgias” and “polymyalgias” as well (“poly-“ means “many”). Experiencing arthralgias and myalgias does not necessarily mean that there is actual arthritis (actual inflammation or damage in the joints) or muscle inflammation. The doctor may not see any evidence of inflammation on examination. If a patient just has achy joints (arthralgias) without having actual inflammation of the joints (arthritis), doctors usually prescribe pain relievers for treatment. These include Paracetamol, non-steroidal anti-inflammatory drugs (NSAIDs; such as ibuprofen and naproxen), or other analgesics such as tramadol.
“I would totally recommend naproxen tablets. I recently got put on them last year in December and I’ve noticed a massive difference to my joint pain; I’m not as stiff, sore or swollen as what I used to be and I feel much more free. I had been taking nearly eight painkillers a day since I was a teenager and now I’m 27 and wish I had been put on naproxen earlier.”
Arthritis
About 50% of people who have SLE will develop actual inflammation of the joints – the medical term for this is arthritis. Fortunately, the arthritis of lupus is usually not crippling or deforming (with the exception of Jaccoud’s arthropathy). Rheumatologists treat lupus arthritis with NSAIDs, steroids, and hydroxychloroquine. Sometimes doctors may need to prescribe stronger immunosuppressant medicines. The goal of treatment is usually to decrease the pain, stiffness, and swelling to acceptable levels.
Tendonitis
Just as lupus can cause inflammation of the joints, it can also cause inflammation of the tendons (tendonitis). Tendonitis usually causes pain around and between the joints of the body, sometimes causing swelling as well. Some examples of tendonitis that can occur in lupus include;
- rotator cuff tendonitis (at the shoulder)
- epicondylitis at the elbow (commonly called tennis elbow and golfer’s elbow)
- flexor tenosynovitis in the palm of the hand (also called trigger finger)
- Achilles’ tendonitis (back of the ankle)
- plantar fasciitis (bottom of the heel)
–
Just as in arthritis, the tendonitis of SLE is treated with NSAIDs, steroids, and hydroxychloroquine, while stronger medications such as methotrexate are used for difficult cases. Resting the tendon to allow the body to heal is one of the most important things to learn to do. An injection with a corticosteroid is also one of the safest and quickest ways to treat tendonitis. Using an ice pack as needed can also help to decrease the severity of the pain from tendonitis.
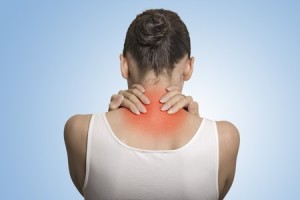 Myositis
Myositis
Myositis refers to inflammation of the muscles caused by a direct attack of the immune system; it can occur in 10% of people who have SLE. Although there may be some achiness in the muscles (myalgias), actual muscle weakness is the more common symptom. If myositis occurs in people who have lupus, doctors usually treat it with steroids but they sometimes use immunosuppressant drugs. If a person just has achy muscles (myalgias) without having actual inflammation of the muscles (myositis), they are treated with pain relievers, such as Paracetamol, NSAIDs, or other analgesics such as tramadol.
Fibromyalgia
Not all joint and muscle pain is due to the inflammation of lupus. About 20% of all people who have lupus will develop a condition called fibromyalgia. Fibromyalgia is due to a chemical imbalance problem of the pain nerves of the body. The treatment of fibromyalgia is completely different from the treatment of lupus arthritis. Instead of using anti-inflammatory medicines, doctors use medicines that reverse the chemical imbalances (such as antidepressants and anti-seizure medicines). Exercise and improving sleep are also important in the treatment of fibromyalgia. Some common symptoms that can point to the possibility of having fibromyalgia include having pain “all over”; having tenderness of the muscles, bones, and skin; headaches; waking in the morning feeling like you did not get much sleep; and feeling tired and fatigued. It is extremely important to identify it as a cause of pain when it occurs to ensure that it is treated appropriately. You can learn more about fibromyalgia from Fibromyalgia Action UK, HERE.
Depression and Anxiety
It can be difficult to convince someone that depression and anxiety disorders can cause pain. People can be resistant to the notion of taking an antidepressant or an anti-anxiety medicine to treat their joint or muscle pain. However, in depression and anxiety disorders, body pain is a very common problem. The treatment of choice is to use medicines that reverse the chemical imbalances that are causing the depression, anxiety, and pain. Pain medicines, anti-inflammatory medicines and steroids should not be used in these cases.
Viral Infections
Viral infections can also cause joint and muscle pain. If you get a fever and have a lot of achiness, it could be due to lupus but you need to see a doctor right away and be evaluated to make sure it is not an infection as well.
Non-Prescription Treatments
Since the vast majority of people who have SLE will get aches and pains due to their lupus, it is very important to learn how to control them. There are things that you can do on your own without relying completely on prescription medicines to gain control;
Joint Protection
 General Joint Protection Techniques;
General Joint Protection Techniques;
- Respect pain; pain should warn you to decrease and avoid certain activities
- Maintain strength and range of motion (see exercise)
- Balance work and rest
- Decrease effort during tasks when using the painful part of your body
- Avoid body positions that cause pain
- Use stronger, larger joints whenever possible
- Avoid staying in one position for too long
- Avoid activities that cannot be interrupted such as standing in long lines or carrying a package for a long distance
–
“A hard thing to do is to get your brain slowed down and to get it to realise what the body can and can’t do!”
“Be kind to yourself. This I learnt in a pain support group. Living with pain 24/7 is tough, so plan weekly treats like seeing a friend for coffee. If you are more housebound try a treat a day like listening to your favourite music or having a favourite biscuit/ice cream.”
Exercise
 A very important part of the treatment of joint and muscle pains is exercise. Due to the discomfort that may occur in lupus, many people are not able to be as active as they were before; they can lose muscle mass, strength, and joint flexibility, preventing them from doing certain activities. This can lead to deconditioning of the muscles of the body and cause even more aches and pains to develop. This becomes a vicious cycle where the pain leads to less activity, less activity causes loss of function and more pain, and so on. Numerous studies show that people who have arthritis who force themselves to exercise regularly actually have less pain overall, develop more muscle mass, are able to do more activities, and have a better quality of life. Not only does exercise help with pain and function, but it has other benefits such as keeping weight under better control, decreasing the chances of developing strokes and heart attacks, and helping with mood in people who have problems with depression.
A very important part of the treatment of joint and muscle pains is exercise. Due to the discomfort that may occur in lupus, many people are not able to be as active as they were before; they can lose muscle mass, strength, and joint flexibility, preventing them from doing certain activities. This can lead to deconditioning of the muscles of the body and cause even more aches and pains to develop. This becomes a vicious cycle where the pain leads to less activity, less activity causes loss of function and more pain, and so on. Numerous studies show that people who have arthritis who force themselves to exercise regularly actually have less pain overall, develop more muscle mass, are able to do more activities, and have a better quality of life. Not only does exercise help with pain and function, but it has other benefits such as keeping weight under better control, decreasing the chances of developing strokes and heart attacks, and helping with mood in people who have problems with depression.
To learn more about exercise in lupus and get tips and advice, please read our previous blog article, ‘Exercising with Lupus’.
“When I was first diagnosed I was prescribed pain killers, but these aren’t ideal in the long term, and I was eager to find better ways to manage my condition. I started off by doing Pilates, where I was taught to breathe into the areas of pain and then imagine the pain leaving my body as I breathed out. As I became more well and fitter, I built up my fitness and gradually introduced other exercise; swimming, cycling, running, boot camp. These days I find that doing exercise keeps my pain under control (I assume by releasing endorphins), and helps me to sleep, not to mention all the other benefits; weight control, cardiovascular benefits and so on. I get lots of aches and pains from doing exercise but it’s a great kind of pain! Obviously I’m lucky in that I’m well enough to be able to exercise, but I do think every one of us can do something; even when I was very unwell I tried to do something. It’s a case of focussing on what you CAN do rather than what you can’t.”
“I’ve found that exercise helps relieve my stiff painful joints. I started going to the gym 18 months ago. In a flare up it is a huge struggle to get to the gym, but it really helps. Also sitting in a Jacuzzi can help with the pain. I also try not to sit for long periods, even when I’m severely fatigued; I get up and walk around for a few minutes before sitting down again. I’m doing strength/weight and conditioning training, my personal trainer has to vary my training according to how my lupus is on the day. I go swimming when I’m mobile enough to get into the pool as you need to climb in via a ladder. I try to do something every day.”
Over-the-Counter Medicines
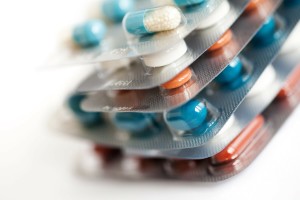 There are medications that are available over the counter that you can safely use to help control pain. It is very important that you read the package instructions thoroughly. Also, check with your doctor first to make sure the medicine is safe to use in light of any other medical problems you may have, and to ensure it is safe to use with your other medications. Never take over-the-counter medicines without doing this first; otherwise there is always the potential risk of drug interactions. NHS Choices has a helpful guide for the type of medicines that you need to treat your type of pain, HERE.
There are medications that are available over the counter that you can safely use to help control pain. It is very important that you read the package instructions thoroughly. Also, check with your doctor first to make sure the medicine is safe to use in light of any other medical problems you may have, and to ensure it is safe to use with your other medications. Never take over-the-counter medicines without doing this first; otherwise there is always the potential risk of drug interactions. NHS Choices has a helpful guide for the type of medicines that you need to treat your type of pain, HERE.
“Recently my doctor put me on vitamin D supplements and it made a huge impact on my fatigue and pain.”
“I find the muscle pain in my legs is worse when I go to bed and am trying to relax. I take tramadol at night and Paracetamol during the day. However I have been using Arnica gel before going to bed and it has greatly improved it.”
Heat and Cold
 Heat and ice are commonly used to treat pain and to reduce swelling, and many people have found them effective. In general, when used sensibly, they are safe treatments which make people feel better and have some effect on pain levels and there are few harmful effects associated with their use. Heat treatments, such as heating pads or warm baths, tend to work best for soothing stiff joints and tired muscles. Heat enhances circulation, delivering nutrients to joints and muscles. It’s good for getting your body ready for exercise or activity. Cold is best for acute pain; it restricts blood vessels, slowing circulation and reducing swelling. It also numbs nerve endings, dulling pain. Various heat and cold treatments can be found HERE.
Heat and ice are commonly used to treat pain and to reduce swelling, and many people have found them effective. In general, when used sensibly, they are safe treatments which make people feel better and have some effect on pain levels and there are few harmful effects associated with their use. Heat treatments, such as heating pads or warm baths, tend to work best for soothing stiff joints and tired muscles. Heat enhances circulation, delivering nutrients to joints and muscles. It’s good for getting your body ready for exercise or activity. Cold is best for acute pain; it restricts blood vessels, slowing circulation and reducing swelling. It also numbs nerve endings, dulling pain. Various heat and cold treatments can be found HERE.
“I use hot water bottles and electric blankets. Damp weather is a killer so I try and take breaks in the winter to warmer climates.”
“A hot shower helps some days when I have joint pains.”
“Hot/cold pads can be helpful. Never put cold one directly on skin, always wrap it in a towel first.”
Stress Reduction
Stress is a factor that can contribute to chronic pain and lupus flares. Advice for managing stress can be found in our previous blog article, ‘Stress Management and Relaxation’.
Complementary Therapies
Acupuncture
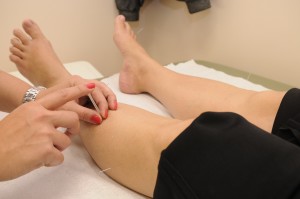 Acupuncture consists of the insertion of very tiny needles into the skin at various points of the body. It may be useful for decreasing the severity of pain. Acupuncture is sometimes available on the NHS, most often from GPs or physiotherapists, although access is limited. Most acupuncture patients pay for private treatment. If you’re being treated by an acupuncture practitioner for a health condition or are considering having acupuncture, it’s advisable to discuss this with your GP and make sure you see an acupuncturist who has proper credentials and training. LEARN MORE
Acupuncture consists of the insertion of very tiny needles into the skin at various points of the body. It may be useful for decreasing the severity of pain. Acupuncture is sometimes available on the NHS, most often from GPs or physiotherapists, although access is limited. Most acupuncture patients pay for private treatment. If you’re being treated by an acupuncture practitioner for a health condition or are considering having acupuncture, it’s advisable to discuss this with your GP and make sure you see an acupuncturist who has proper credentials and training. LEARN MORE
“I tried a chiropractor but the pain was too much and couldn’t complete the course. Chinese Medical Acupuncture – six-week course was good for me.”
“The only treatment I have found that gave me any respite was Chinese medical acupuncture. I had a six-week course, but I can’t afford this anymore as I can’t work.”
Prayer
The power of prayer has not been formally studied in lupus, but it has been studied in other medical conditions. A review of prayer studies in 2000 showed that 57% of the studies had a positive treatment effect. Therefore, prayer should be encouraged in people who use prayer in their religious beliefs.
Meditation
 Meditation refers to a large group of practices used in religion as well as for secular (non-religious) purposes to change a person’s inward mode of consciousness. It often involves resting quietly, often with eyes closed, concentrating on breathing, and sometimes involves saying words repeatedly (called a mantra). In complementary medicine, it is used to increase calmness and physical relaxation, to improve psychological balance, to cope with illness, or to enhance overall health and well-being. Studies have shown its usefulness for the pain and tenderness of rheumatoid arthritis.
Meditation refers to a large group of practices used in religion as well as for secular (non-religious) purposes to change a person’s inward mode of consciousness. It often involves resting quietly, often with eyes closed, concentrating on breathing, and sometimes involves saying words repeatedly (called a mantra). In complementary medicine, it is used to increase calmness and physical relaxation, to improve psychological balance, to cope with illness, or to enhance overall health and well-being. Studies have shown its usefulness for the pain and tenderness of rheumatoid arthritis.
One form of meditation which is now widely practiced and recognised for various benefits to health and wellbeing is mindfulness. You can learn more about this practice HERE.
Hypnotherapy
Hypnotherapy (hypnosis) is a type of relaxation therapy where the hypnotherapist guides the individual into a heightened state of relaxation along with an increased focus in attention. It has been used for anxiety, smoking cessation, weight control, and to help decrease pain. LEARN MORE
“I’d thoroughly recommend hypnotherapy for stress or pain relief. It can be done either face to face or by listening to mp3 recordings at your leisure. It’s relaxing, non-invasive and yet very effective. There are many different types of recordings out there, some good and some, quite frankly, just awful. It really depends on what each person needs.”
Aromatherapy
 Aromatherapy uses the inhalation of essential oils from trees, herbs, and flowers to promote health and well-being. Examples of oils used include chamomile, lavender, geranium, cedar and lemon. Proponents of this form of therapy suggest that they can help with mood, sleep, decrease stress, and possibly help with pain and nausea. LEARN MORE
Aromatherapy uses the inhalation of essential oils from trees, herbs, and flowers to promote health and well-being. Examples of oils used include chamomile, lavender, geranium, cedar and lemon. Proponents of this form of therapy suggest that they can help with mood, sleep, decrease stress, and possibly help with pain and nausea. LEARN MORE
“I find aromatherapy and massage helps me cope with joint pains.”
Massage
 Massage involves the physical manipulation of the body tissues by a massage therapist to decrease pain, anxiety, stress, and to improve “circulation”. There is some emerging evidence that it may be beneficial for depression, anxiety disorders, and to help decrease pain severity. Make sure that your massage therapist is licensed and fully aware of your medical conditions. LEARN MORE
Massage involves the physical manipulation of the body tissues by a massage therapist to decrease pain, anxiety, stress, and to improve “circulation”. There is some emerging evidence that it may be beneficial for depression, anxiety disorders, and to help decrease pain severity. Make sure that your massage therapist is licensed and fully aware of your medical conditions. LEARN MORE
“I have had all sorts but I do like Bowen therapy; it helps the pain that’s there all the time.”
“I’ve had a few massages to try and help with pain, but it brings on a flare or I am in pain for days after.”
Reiki
Reiki is a Japanese healing art developed in the 1920s by a Japanese Buddhist. Its proponents believe that an invisible healing energy can be transmitted from the healer to the patient through intuition by placing the hands on certain parts of the patient’s body. It can also be practiced at a distance from the patient as well. There are no studies of its use in lupus. A 2011 study in cancer patients suggested that it may be helpful for pain, sleep, relaxation, anxiety and improving one’s sense of overall well-being. LEARN MORE
Reflexology
 Reflexology is a type of massage where pressure is applied to your feet and hands. There is some evidence that reflexology can help you to relax and cope with stress and anxiety, help relieve pain and help lift mood and give a feeling of well-being. LEARN MORE
Reflexology is a type of massage where pressure is applied to your feet and hands. There is some evidence that reflexology can help you to relax and cope with stress and anxiety, help relieve pain and help lift mood and give a feeling of well-being. LEARN MORE
“I have just had my first session of reflexology and for the first time in two years I felt good; I was relaxed and my head fog was gone until the next day which was brilliant! Also I slept for ten hours which I can’t remember the last time I slept that long. I can’t wait for my next session!”
Yoga
 Yoga is an ancient form of exercise that focuses on strength, flexibility and breathing to boost physical and mental wellbeing. Yoga is now commonplace in leisure centres, health clubs, schools, hospitals and surgeries. There’s some evidence that regular yoga practice is beneficial for people with high blood pressure, heart disease, aches and pains (including lower back pain) depression and stress. LEARN MORE
Yoga is an ancient form of exercise that focuses on strength, flexibility and breathing to boost physical and mental wellbeing. Yoga is now commonplace in leisure centres, health clubs, schools, hospitals and surgeries. There’s some evidence that regular yoga practice is beneficial for people with high blood pressure, heart disease, aches and pains (including lower back pain) depression and stress. LEARN MORE
“I’ve been attending Yoga classes for almost two years and I can say I have the best night’s sleep following my class.”
Additional NHS Services
Hospital Pain Clinics
 There are around 300 pain clinics in the UK. Most are in hospitals and have teams of staff from different medical areas, including occupational therapists, psychologists, doctors, nurses and physiotherapists. They all work together to help people with pain.
There are around 300 pain clinics in the UK. Most are in hospitals and have teams of staff from different medical areas, including occupational therapists, psychologists, doctors, nurses and physiotherapists. They all work together to help people with pain.
Pain clinics vary but usually offer a variety of treatments aimed at relieving long term pain, such as painkilling drugs; injections; hypnotherapy and acupuncture.
You will need to be referred to a pain clinic by your GP or hospital consultant.
“I’m heading back shortly to the pain management clinic for a second round of acupuncture. I finally got a cocktail of meds that seem to work. It does take time as what works for one may not work for another. Both pain consultants and my primary medical care team have decided physiotherapy is not a working option for me. I have found the counselling side of pain management to be very effective. It was important to find someone who believes that mental health can be affected by pain levels and not just the other way round (i.e. It’s all in your head). I’d be lost without the lovely nurse in our pain management clinic.”
“I have had severe back pain for a long time. I was eventually referred to a pain management consultant who did a spinal injection for me which has really eased my pain and I only need one every six months. It has helped me to reduce my medication. I also have acupuncture once a month which I find really helps. I was referred by my GP on the NHS, then my physio went private so I have continued to see her on a private basis.”
Pain Management Programmes
Pain management programmes are a series of sessions, for groups of 6-8 people, aimed at teaching you how to live with your pain. Instead of treating your pain, you learn to cope with it and, research shows, can expect to enjoy a better quality of life, sleep and mobility afterwards. It should be noted that the techniques practiced in pain management programmes may not be effective for everyone.
Some hospital pain clinics offer pain management programmes, and some are held within GP surgeries.
As with pain clinics, you will need a referral to join a pain management programme from a GP or hospital specialist.
“I was fortunate enough to be referred to attend a chronic pain self-management three-week residential course at Bath Rheumatic Diseases Hospital years ago which helped me with coping strategies etc. I think you have to be open minded as self-management doesn’t work for everyone…you’ve got to be in the right frame of mind to accept the change and move forward.”
“I was referred to a pain management course. I have to say I found the whole thing a waste of time which was a shame. There was a session with a nurse discussing the medication everyone was taking and advising everyone to either cut down or stop but when I said about Plaquenil (hydroxychloroquine) she hadn’t even heard of it. If I am honest I felt the group was based around pain from injuries rather than a long-term illness.”
Occupational Therapy
Occupational therapy provides support to people whose health prevents them doing the activities that matter to them. An occupational therapist can identify strengths and difficulties you may have in everyday life and will help you work out practical solutions.
They can work with you to identify goals that can help you maintain, regain, or improve your independence by using different techniques, changing your environment, and using new equipment.
More information about Occupational Therapy and how it can help can be found in this guide from Arthritis Research UK, HERE.
Information about how you can access Occupational Therapy can be found HERE.
“I have an orthopaedic office chair. I have changed my car to an automatic and a 4×4 so it is easier to step in and out of. We are considering a walk-in shower rather than a step into the bath/shower which we currently have. I also have a cleaner and ironing lady.”
Additional Reading
NHS Choices – Living with Pain
Chronic Pain – A Self Help Guide
The Pain Toolkit
Pathway through Pain
Pain Concern
Action on Pain
Pain UK
Away with Pain
Pain Relief Foundation
Change Pain
***Please note that this article is written for informational purposes only and should not be a substitute for professional medical advice or treatment. Do not delay seeking or disregard medical advice based on information here. Always seek the advice of your local family physician or other qualified health professional before starting any new treatment or making any changes to existing treatment. It is also advisable to consult a medical professional before making any changes to diet or starting alternative remedies, which may interact with other medications.***
Thank you so much to everybody who submitted their tips and experiences for this month’s topic. We’re sorry if we weren’t able to use your comment in the article this time.



 ©2024 LUPUS UK (Registered charity no. 1200671)
©2024 LUPUS UK (Registered charity no. 1200671)